Massage often gets a bad rep in the world of rehabilitation or physiotherapy. If you’re someone who follows the latest spotlights and trending fitness/rehabilitation influencers on Instagram or Twitter, you might have come across ‘discussions’ (which look very similar to arguments and Internet fights!) where the therapeutic benefit of massage therapy is fought over and debated — often with the eye-catching conclusion that “Massage is over-rated”, “Massage is unlikely to help your pain for the long-term”, or even the well-intentioned “Movement is Medicine, not lying on a bed and getting massaged”!

While we get the point — we just want people to start moving, getting active, and live a healthier lifestyle without relying on passive care — I think that we’ve thrown the baby out with the bathwater. If massage absolutely didn’t work, there wouldn’t be a need for registered massage therapists (RMT), nor their often two-year full-time courses, nor their acknowledgement and involvement in many Health Care Professions Act internationally such as in the US, Canada, and Australia.
While not a panacea for relieving every possible body ache and pain out there, massage (or often called soft tissue therapy) has many other positive effects that are scientifically backed to provide therapeutic benefits… Provided it is used at the right time for the right person.
How does massage help — scientifically?
If we take a stroll through the literature and look at what a recent systematic review says about massage, we find that the body of evidence generally agrees that massage therapy improves various patient-reported functional outcomes among populations experiencing musculoskeletal pain (e.g. back pain, neck pain, etc).
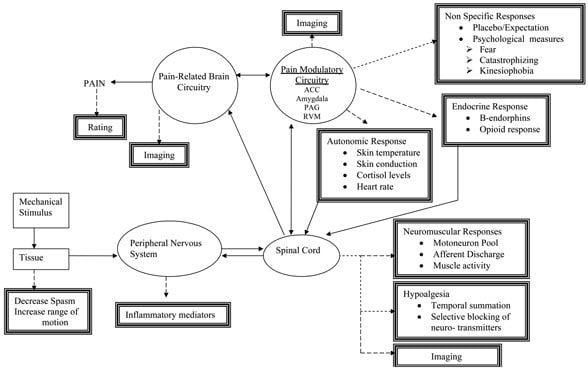
Big picture. Short summary. Massage therapy, or anything involving touch/pressure, affects the neurological pathways between the brain and the target site.
Our muscles contain structures sensitive to pressure and stretch (mechanosensitive structures). When activated through massage (that’s pressure and stretch on the muscles!), it allows for signalling to occur, inducing relaxation and reducing pain signals.
A real life case study…
Patient X* came in last year complaining of a 12-year long history of neck pain and headaches. She had been going for regular chiropractic adjustments twice monthly to temporarily relieve her pain as, due to health conditions, she was not able to sustain a physical activity regimen.
Due to the period of COVID-19 lockdown and an even greater reduction in activity levels, she began to develop constant headaches everyday for 2 months which affected her ability to work in front of the computer. Painkillers were also part of her daily regimen, and sometimes the headaches would progress into migraines that kept her in bed, to the point where her regular chiropractic adjustments were only providing relief for a day.

Trust me when I say that our first consultation was NOT the most pleasant of encounters! And she really couldn’t be blamed, because who would be cheerful when you’ve been experiencing a constant head and neck pain for 2 months and someone is trying to ask you questions and get you moving in ways that you wouldn’t normally want to be doing? (That’s our initial consultation)
-
Assessment
The assessments ruled out any serious matters contributing to her headache, such as high blood pressure (controlled with medication, normal on the day itself), night sweats, sudden weight loss, pain worsening in the early mornings or nights (possible indication of a space-occupying lesion). A lack of any paresthesias, referred/radiating pain, and negative nerve tension tests minimised the possibility of a slipped disc or nerve issue.
What was left was the positive findings of hyperactivity and sensitivity of all the muscles around the neck and shoulders — commonly a protective mechanism from constant pain — and poor joint mobility of the cervical region. Our working diagnosis was cervicogenic headaches, whereby the excessive stress around her neck and shoulders was causing her to develop headaches developing into migraines on high-stress days.
-
Treatment
So, what can be done for those who can’t exercise, are experiencing a moderate to severe type of headache constantly, and are wanting an alternate option to reduce her painkiller usage and return her high-stress work to a more functional capacity?
That’s where sports massages can come in, especially for those experiencing a high level of muscle tension that contributes to their symptoms.

She came in regularly for sports massages for 6 months; initially once a week, and then dropped the frequency to once every two weeks, and subsequently even further to coming as and when needed. The soft tissue therapy focused a lot on targeting the muscles around her neck (suboccipitals, scalenes, SCM) and the midback (e.g. trapezius, rhomboids, levator scapula), and sometimes even further down to the latts.
There were also sessions where lymphatic drainage was done as a form of soft tissue therapy, which can come in really beneficial during the days she was experiencing extra sensitivity and pain. The biochemical substances causing pain which are released during a migraine or headache flare can be manually guided to move away from already sensitive areas (Discussed in papers from 1989, up until 2016 where researchers found that a combination of massage and lymphatic drainage significantly reduced migraine attack frequency over a period of 4 weeks).
Towards the end of the 5th month and going into the 6th month, she was back to full force at work, minimal occurrence of headaches that she was able to self-manage herself, and a much happier outlook on life. I’ll quote her — “I haven’t felt this level of nearly no pain in the past decade.” And while the addition of a physical exercise programme may have hastened her progress, this gives us a treatment for those whom it may not be possible.
Conclusion

Massage has its time and place.
While strength, function, and a healthy lifestyle is always advocated for, how does one get started on all those things when pain is at the forefront of a patient’s condition?
Trained as professionals in the field of muscles, joints, and nerves, we utilise clinical reasoning and equip ourselves with as many logical and effective tools in our toolbox so that we are ready to treat the individual where they are at.
And sometimes, that can look like massage and soft tissue therapy before we bring out movement, function, and strength.
A note to physiotherapists: You DON’T need the ability to massage to be a good physiotherapist. Instead, you need the ability to rationalise and choose when it is needed and when it isn’t, and how to listen to what the patient is really telling you.
——————————————
*Name & details undisclosed for privacy purposes.
[This article was written by Hannah, our physiotherapist who specialises in sports massage for those with chronic pain.]
Sources:
- Bialosky, J. E. et al. (2009) The mechanisms of manual therapy in the treatment of musculoskeletal pain: a comprehensive model. Manual therapy, 14(5), 531–538. https://doi.org/10.1016/j.math.2008.09.001
- Bishop, M. D. et al. (2015) What effect can manual therapy have on a patient’s pain experience? Pain management, 5(6), 455–464. https://doi.org/10.2217/pmt.15.39
- Happe, S. et al. (2016) The efficacy of lymphatic drainage and traditional massage in the prophylaxis of migraine: a randomized, controlled parallel group study. Neurological sciences: Official journal of the Italian Neurological Society and of the Italian Society of Clinical Neurophysiology, 37(10), 1627–1632. https://doi.org/10.1007/s10072-016-2645-3
- Trettin H. (1989) Die manuelle Lymphdrainage in der Migränebehandlung–ein pathophysiologisches Erklärungsmodell [Manual lymph drainage in migraine treatment–a pathophysiologic explanatory model]. Zeitschrift fur Lymphologie. Journal of lymphology, 13(1), 48–53
- Waters-Banker, C. et al. (2014) Investigating the mechanisms of massage efficacy: the role of mechanical immunomodulation. Journal of athletic training, 49(2), 266–273. https://doi.org/10.4085/1062-6050-49.2.25
